July 2018
Feline Tularemia
By Drs. Argine Cerezo, Timothy Walsh and Mike Moore
Tularemia, also known as rabbit fever, is a zoonotic disease caused by the bacterium Francisella tularensis. This disease is considered one of the most infectious pathogens known in human medicine with an extremely low infective dose.2 Rabbits and rodents are very susceptible to infection and may die in large numbers during outbreaks.2 Cats, the most commonly affected domestic species, acquire this disease as a result of interaction with or ingestion of wildlife reservoirs, their vectors, or from exposure to a contaminated environment. Additionally, the disease can be transmitted by ticks, biting flies, penetrating injuries, water exposure, contaminated food, and aerosols.2 The disease tends to be seasonal, with higher incidences in late spring, summer and early autumn, probably due to the availability of the tick vector. 1
Clinical signs are often peracute (e.g. animal found dead) or infected animals may present with fever, marked depression, lymphadenomegaly, hepatomegaly, splenomegaly and/or oral ulcers. 2,3 The Kansas State University Diagnostic Laboratory (KSVDL) has confirmed at least six tularemia cases since March 2018, making this relatively common within the State of Kansas.
History/ Clinical Signs: An 18-month-old intact male domestic short hair cat presented with a history of acute neurologic signs and progressive ataxia over a 24-hour period. Due to human exposure, the cat was euthanized and submitted to KSVDL for rabies testing and necropsy.
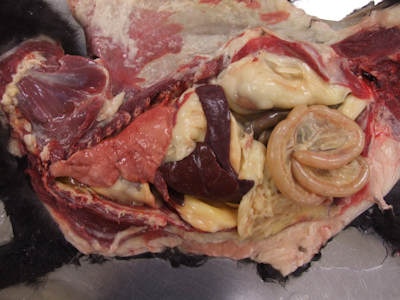
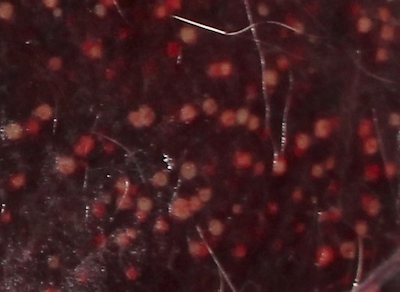
Diagnostics: At necropsy approximately 50 percent of the spleen and liver contained multifocal, 1 mm diameter, well demarcated, round, tan nodules. Figures 1 and 2. No other significant gross lesions were found. Histologically, abruptly disrupting the parenchyma of the spleen and liver, there were multifocal, scattered areas of necrosis affecting both white and red pulp. Figure 3.
The gross lesions were consistent with a necrotizing splenitis and hepatitis, classically associated with Tularemia or Plague. Since both of these diseases are reportable and potentially zoonotic, a sample of spleen was submitted for bacterial culture. Brain stem and cerebellum were test negative for rabies. Culture of the spleen at KSVDL was suspect for Francisella tularensis, and was confirmed by PCR and culture at the Centers for Disease Control and Prevention.
Take Home Message: Tularemia is an endemic, dangerous, easily-transmitted zoonotic disease. Any reported “healthy” cat (outdoor or indoor) with a peracute/acute, fatal disease should be suspected of Tularemia. Due to the potential zoonotic risk necropsy on-site should not be attempted, whenever possible. (Because of this risk, KSVDL pathologists necropsy Tularemia suspect cases in a biological safety cabinet.) It is recommended for these cases that the entire carcass be sent immediately to a diagnostic laboratory where confirmatory testing can be performed. (Please call the lab before submitting the carcass to communicate that a Tularemia suspect will be arriving.) The most common clinical signs are acute death, or fever, lethargy, and marked lymphadenomegaly.
This case did not present with the severely enlarged submandibular lymph nodes and rabies was a definite rule out due to reported neurologic signs. It reminds us of the importance of proper personal protective equipment when handling patients. For antemortem diagnosis in suspect Tularemia animals, culture of lymph node aspirates is the recommended diagnostic test.
If you have questions, please contact KSVDL Client Care at 866-512-5650 or clientcare@vet.k-state.edu.
References:
- Greene, C. E. (2013). Infectious Diseases of the Dog and Cat. 4th ed. Elsevier Health Sciences.
https://www.cdc.gov/tularemia/ - J.F. Zachary (2016) “Pathologic basis of Veterinary Disease, 6th ed.” Elsevier, (Vol. 2) p.184-185. ISBN-13: 978-0323357753